In these scenarios, lung auscultation and pulse oximetry provided the EMTs with insufficient ventilatory information, leading to patient deterioration. It can help monitor patient response to bronchodilator and non-invasive positive pressure ventilation treatment. Capnography could also reveal impending complications such as cardiovascular collapse or pneumothorax. If the EMT had access to end-tidal capnography, it may provide clues for the etiology of the patient’s respiratory distress. 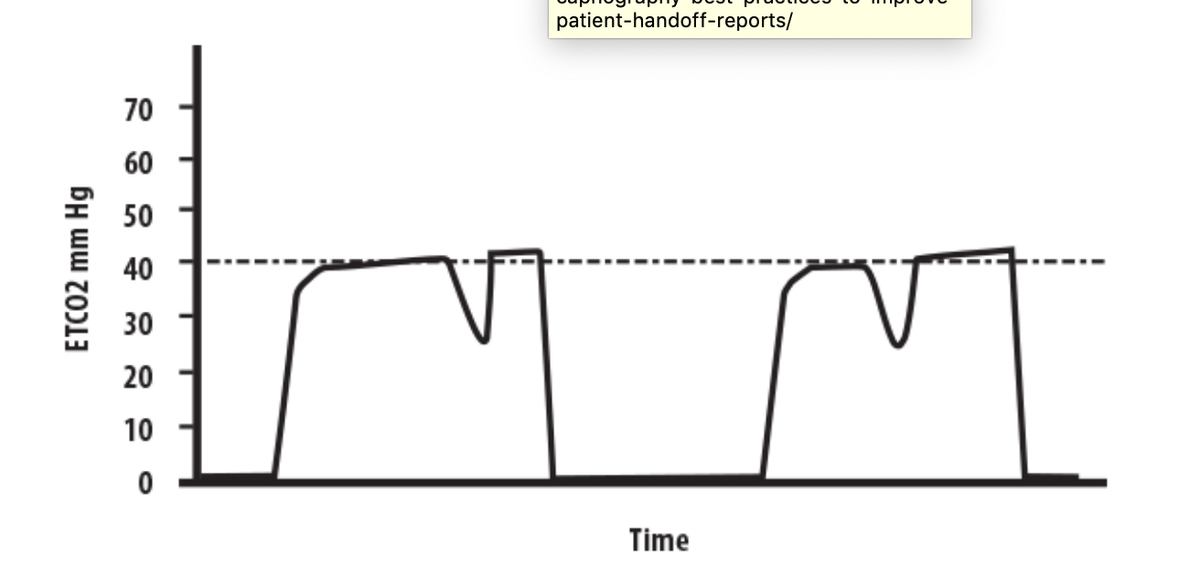
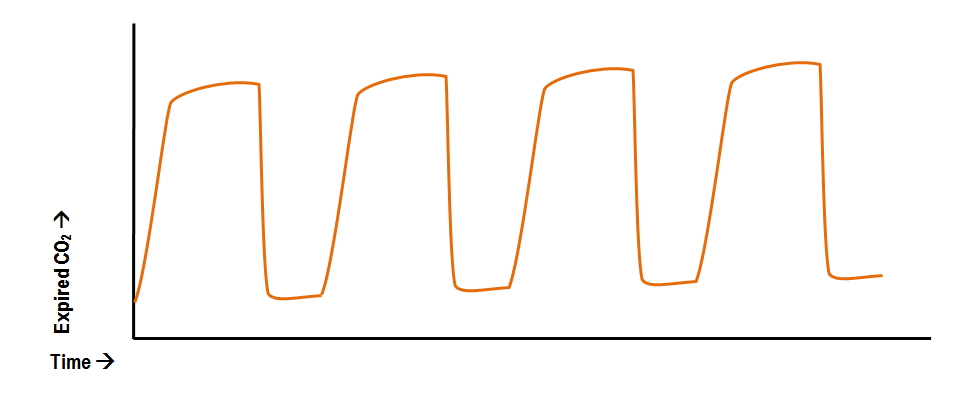
Throughout transport, the patient continues to experience respiratory distress, and their SpO2 slightly increases from baseline. The EMT administers an albuterol treatment and places the patient on CPAP. Due to the patient’s medical history, physical presentation, and vital signs, the EMT concludes the patient is experiencing a COPD exacerbation. Furthermore, they would have observed that ventilating the patient more forcefully was not improving alveolar gas exchange, reducing the likelihood of continued overventilation and patient injury.Īn elderly patient is experiencing difficulty breathing. If the EMT had access to end-tidal capnography, they would have known whether they were adequately ventilating the patient. Although the EMT sees adequate chest rise and fall, the pulse oximeter reads “low.” Unsure if they are ventilating the patient adequately, the EMT begins squeezing the BVM more forcefully and ventilating the patient at a faster rate, inducing barotrauma and gastric inflation. Respirations are inadequate, so one EMT begins positive pressure ventilations while the other cools the patient. Monitoring Positive Pressure Ventilation:Ī patient is unresponsive due to heat stroke. If the EMT had access to end-tidal capnography, they would have noted the patient’s drop in respiratory rate and depth almost immediately, minutes before the delayed notification from the pulse oximeter and falling heart rate. The patient’s heart rate begins to drop, and the EMT promptly begins positive pressure ventilations. Upon auscultation, they are not sure if they can actually hear any lung sounds over the driving noise. The EMT begins to count respirations, and finds the chest rise and fall very shallow. The EMT switches to a non-rebreather with an airway adjunct, and increases the amount of oxygen, but the SpO2 continues to drop. On route to the hospital, the EMT notices that the patient’s SpO2 is slowly dropping. Pulse oximetry reads 92%, so the EMT manually opens the airway and places the patient on supplemental oxygen via nasal cannula. Prior to leaving the scene, normal pulse rate and adequate respiration rate and depth are confirmed. Here are three quick scenarios demonstrating the potential benefits of waveform capnography during common EMT-level interventions.Īn unresponsive patient has been loaded onto the ambulance by EMTs. Once trained in capnometry interpretation, EMTs would gain valuable information that other vital signs cannot quickly provide. Lower respiratory system and V/Q abnormalities cause deviations from the expected “table shape” that are easily recognizable and clinically useful. In a healthy patient, this physiological process produces the usual “table-shaped” waveform with plateau readings of 35-45 mmHg. As exhalation continues, the CO2 partial pressure plateaus, and then returns to baseline upon inhalation. During initial exhalation, the CO2 partial pressure rises sharply as CO2 rich gas arises from the alveoli. During inhalation, the ETCO2 sensor reads a baseline CO2 partial pressure. A small end tidal carbon dioxide (ETCO2) sensor is placed at the patient’s nose or mouth. Waveform capnography is a non-invasive tool that provides a quantitative measure of expired CO2 throughout the respiratory cycle. Here, the benefits of waveform capnography to EMTs and their patients will be discussed. The limitations of lung auscultation and pulse oximetry can be addressed by the introduction of waveform capnography to the EMT scope of practice (Brandt 2010). However, in order to evaluate ventilation and perfusion, EMTs must currently rely on lung auscultation and pulse oximetry - both of which have critical limitations (Brown et al., 1997 Chan et al., 2013 DeMeulenaere 2007). The Benefits of Waveform Capnography for Patient CareĪs discussed in Part 1, under the National EMS Scope of Practice Model (2019), EMTs are expected to initiate several critical airway and breathing interventions for a variety of medical and traumatic conditions.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
